By Ethan Harned and Lena Dougherty
With the goal of ensuring all in Uganda have access to palliative care services, the Palliative Care Association of Uganda (PCAU) has partnered with multiple civil society organizations and conducted focus groups and surveys to evaluate the accessibility of palliative care services for persons with disabilities (PWDs). The results of this work will inform PCAU on where they should focus their efforts going forward.
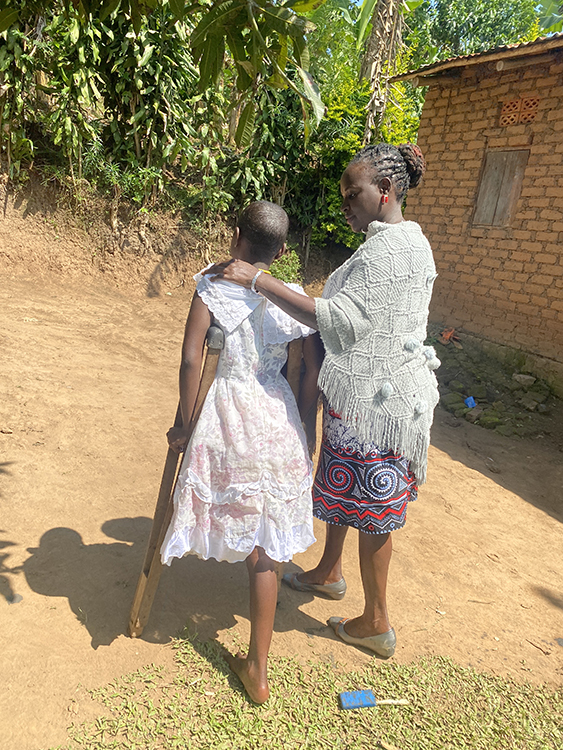
While palliative care interventions continue to be impactful, the unique needs of PWDs during these interventions are often overlooked. The prevailing assumption that these patients, like other palliative care patients, can be adequately supported within routine practice standards, fails to acknowledge the multifaceted challenges they encounter. PWDs, who have long endured prejudice, bias and devaluation, face heightened vulnerability when utilizing palliative care services. Consequently, it is imperative to undertake an honest and thoughtful reevaluation of the standard model of palliative care in Uganda to address these unmet needs.
According to a 2019 report from the Uganda National Bureau of Statistics, approximately 14% of the Ugandan population over five years of age lives with at least one disability. The prevalence of disability in Uganda increases with age from 6.3% for children 5 – 17 years old to 61.5% for those over age sixty. With these statistics, accessible palliative care is even more important to consider. This article aims to shed light on the challenges PWDs face in Ugandan palliative care settings and the importance of recognizing and accommodating the specific requirements of these patients.
When attempting to access health centers, PWDs face significant obstacles. The challenge of movement to and from health centers is due to not only the mobility disability itself, but also inadequate means of transportation and distance to healthcare facilities. This challenge is only exacerbated if a PWD lacks an appropriate mobility aid. Challenges in accessing services continue to present themselves during treatment due to the lack of accommodating infrastructure of health centers, such as inaccessible entryways, hallways, rooms, beds and appropriate toilet facilities.
Once a PWD arrives at a health center, they face challenges in receiving care due to a number of communication barriers. Many healthcare workers lack education on the proper treatment of PWDs and how to manage their care. This, coupled with a lack of sign language interpreters and braille texts, prevents those living with visual or hearing impairments from being able to express themselves well to their providers. In addition, healthcare workers often speak directly to a patient’s caretaker rather than the patient themselves, which can lead to miscommunications that prevent PWDs from adhering to the recommended practices for managing lifelong illness using palliative care.


Beyond the physical reasons listed above as to why a PWD is unable to access a health center, there are many sociocultural factors preventing a PWD from receiving palliative care services. Research and testimonials from PCAU’s focus group discussions revealed that most PWDs are economically poor. Many are prevented from receiving any formal form of education due to the stigmatization of their disability. Those who have received an education face discrimination in the workplace that prevents them from retaining employment.
This economic hindrance makes it difficult for PWDs to afford transportation or purchase necessary aids that allow them to access palliative care services. Due to the stigmatization of their disability, many do not receive any form of support from their families or communities, which only serves to put them into a more dire position.
The stigma a PWD faces has a significant impact on how aid is distributed or outreach is conducted as it often overlooks PWDs. In PCAU’s focus groups, participants had little knowledge of what palliative care services were, how they could benefit, or what resources were available to them within their communities. As a result, PWDs are unlikely to make any formal contact with palliative care providers in their districts.
It is overwhelmingly evident that PWDs in Uganda lack access to proper palliative care services. This disparity has persisted for a variety of reasons. One of those reasons is the lack of research in Uganda, and more broadly Sub-Saharan Africa, on the utilization and accessibility of palliative care services for PWDs. Moving forward, it is important that these topics be evaluated as new programmes to support PWDs emerge across the continent. Increased interest through academic research and discourse will ensure PWDs are properly advocated for and supported in Uganda.
 Palliative care organizations must evaluate their services to assess how accessible they are to PWDs. Outreach efforts by these organizations must be adjusted to target PWDs in the communities in which they work. This is the current appeal by the Palliative Care Association of Uganda. These outreach efforts must also sensitize their communities to the needs of PWDs and how they could benefit from palliative care services.
Palliative care organizations must evaluate their services to assess how accessible they are to PWDs. Outreach efforts by these organizations must be adjusted to target PWDs in the communities in which they work. This is the current appeal by the Palliative Care Association of Uganda. These outreach efforts must also sensitize their communities to the needs of PWDs and how they could benefit from palliative care services.
In working to reduce these disparities facing PWDs in accessing palliative care services, PCAU worked closely with Esther Namara, a social worker. She worked for PCAU for six months to further PCAU’s efforts to bring palliative care services to all PWDs. Due to funding challenges, PCAU has not been able to employ Namara full-time. Namara had the opportunity to share PCAU’s successes thus far in making palliative care more inclusive to PWDs at the 2023 Uganda Cancer and Palliative Care Conference. With appropriate funding, PCAU could offer Namara a full-time position and work to make every palliative care unit in Uganda disability-inclusive.
To conclude, the rights to healthcare of PWDs are not being adequately respected. It is crucial to acknowledge and address the specific needs of PWDs. Through careful examination of the palliative care services being offered in Uganda and proper resource mobilization, disparities in the current care model can be eliminated, and PCAU will be one step closer to their goal of ensuring all in Uganda have access to palliative care services. By doing so, PCAU can ensure that everyone in Uganda receives the utmost support, compassion, and generosity throughout their lives, regardless of who they are.
